In an ideal world, patients would pay the full amount at time of service every time. But that’s not always possible, so you will inevitably end up sending billing statements. If you have to bill a patient, make it as easy for them to pay as possible so that you don’t have to spend time and effort on collections.
You know your patients, and you understand how to best communicate with them. With QuickBill Premium, you get a chance to put that expertise to use to send patients their statements the way that best suits them so that they’re more likely to pay promptly.
To select the delivery method for statements:
- Generate your billing statement batch as you normally would and click the Electronic Submission button.
- In the Verify Statements to Send window, look at the delivery method for each guarantor’s statement.
- Select the option(s) that best suit each guarantor:
- Select Mail to send the statement to the QuickBIll clearinghouse to be printed and mailed.
- Select Email to send a link to view the statement online via an email message.
- Select Text to send a text message containing a link to view the statement online.
- Select any combination of the options to send the statement to the patient in multiple ways: through mail, email, or text message.
- Clear all options to skip that guarantor and not send the patient a statement in this batch.
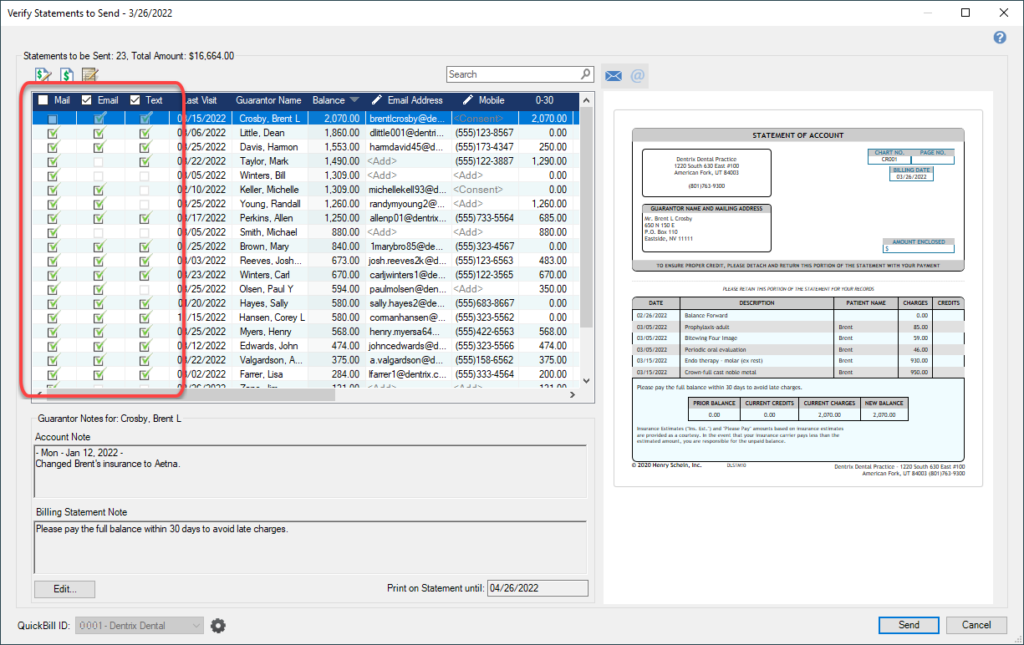
- When you’ve reviewed and selected the delivery method(s) for each account, click Send.
Take control of your billing and collection processes with Dentrix QuickBill Premium. By sending statements via mail, email, and /or text message you can speed up payments, cut costs, and take the frustration out of billing for both your team and your patients.
Learn More
Watch our on-demand webinar titled Collect Payment Faster with Online Patient Payments to learn more about how using QuickBIll Premium can benefit your practice.
Visit the QuickBill Premium Quick Start page for links to videos and articles about how to perform tasks related to generating and sending billing statements via QuickBill.

